A PATIENT’S GUIDE TO NEUROPATHY Michael Zapf, DPM, MPH, FACFAS Burning, tingling and painful feet are one of the most common reasons patients visit my office, not surprising since 2 to 10 million people in the United States have these symptoms. In the recent past, David complained that his […]
Rachel
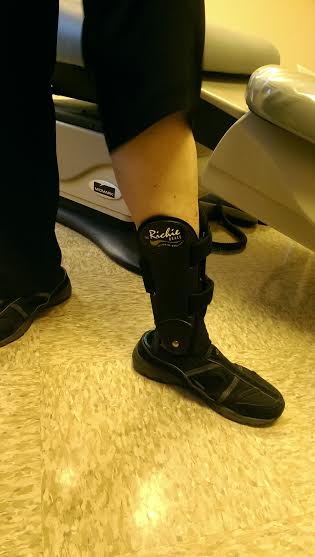
Another brace success story…. One of our patients, S.J.A. is an avid walker who noticed her left ankle becoming more and more unstable. She tried changing her shoes and wearing orthotics, but her ankle still felt like it needed more support. She felt her instability was preventing […]
An article posted on Healthgrades indicated that several common anti-inflammatory medications are and have been associated with high blood pressure, heart disease and stroke. Vioxx is the poster child for these medications and has already been taken off the market. The more common medications that can cause these complications are ibuprofen […]
*Compression stockings* Many people need to wear compression stockings to assist blood and other fluid circulating in the legs to get back to the heart. A lot of times, patients are turned off by these garments because they are very difficult to put due to how tight they need to be. In […]
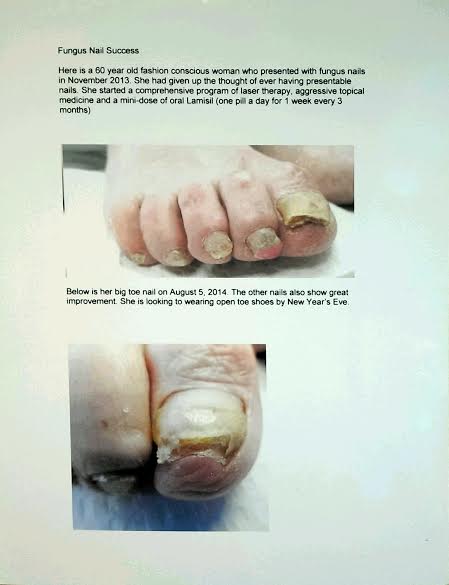
“You guys sell nail polish?” This is a question heard daily in our offices. Not only do we sell nail polish, but we sell Dr. Remedy nail polish, which is made from a blend of wheat protein, tea tree oil, garlic bulb extract and lavender. There is no formaldehyde, formaldehyde […]
Safety Announcement [8-15-2013] The U.S. Food and Drug Administration (FDA) has required the drug labels and Medication Guides for all fluoroquinolone antibacterial drugs be updated to better describe the serious side effect of peripheral neuropathy. This serious nerve damage potentially caused by fluoroquinolones (see Table for a list) may occur soon […]
Our own Drs. Zapf, Payne and Benson are members of Choice Health Associates. This is a group of more than 200 local doctors who have banded together to offer the best in medical service to the patients from Calabasas to Moorpark and Camarillo. We all agree to see referrals as […]
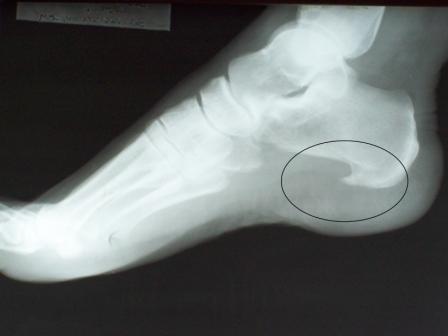
Maybe Heel Spurs Are Important For years you foot doctor has been telling all you heel pain patients that heel spurs are just an incidental finding on an x-ray and not a cause of pain. That opinion may have to change. A recent article in Foot and Ankle Specialist (April […]